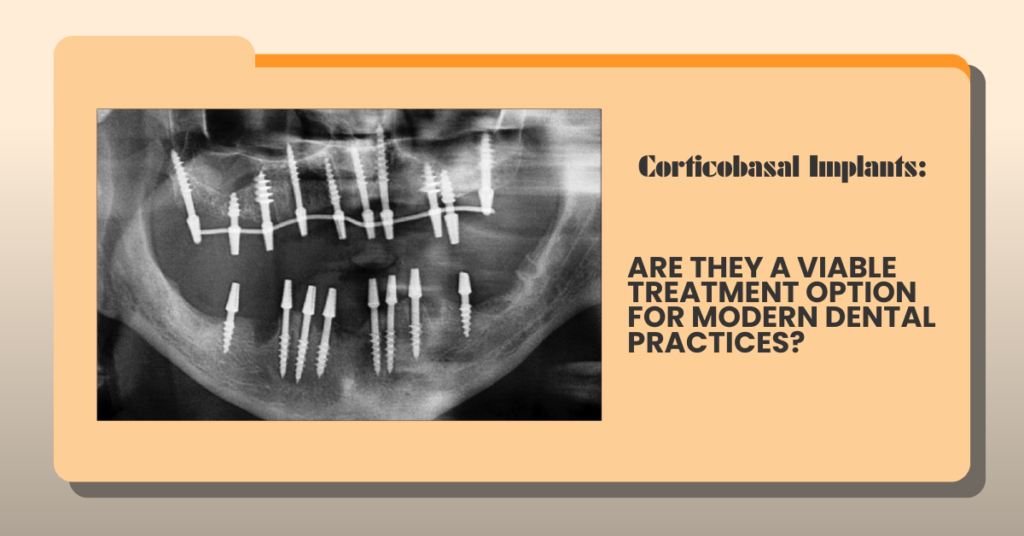
Implant dentistry has evolved rapidly over the last two decades. What was once considered a complex, multi-stage procedure has transformed into a predictable and patient-friendly solution for missing teeth. Yet, one challenge continues to test even experienced clinicians — managing implant cases with compromised bone.
As dental practices see an increasing number of patients with advanced bone resorption, systemic conditions, or limited tolerance for prolonged treatment timelines, clinicians are beginning to revisit alternative implant concepts. One such approach that has gained attention is corticobasal implantology.
This article explores corticobasal implants from a clinical decision-making perspective, helping dentists understand where they fit, where they don’t, and why the discussion matters today.
The Clinical Challenge Facing Implant Dentists Today
Modern dental practices are no longer dealing with ideal textbook cases alone. Common challenges include:
Severe alveolar bone resorption
Patients unwilling or unsuitable for bone grafting
Demand for faster functional outcomes
Financial constraints affecting treatment acceptance
Medically compromised or elderly patients
While conventional endosseous implants remain the gold standard, they often rely heavily on adequate bone volume, grafting procedures, and delayed loading protocols. In many real-world scenarios, this can lead to treatment drop-offs or prolonged rehabilitation.
This gap between clinical ideals and patient realities is what drives interest in alternative implant philosophies.
Understanding Corticobasal Implants (At a Conceptual Level)
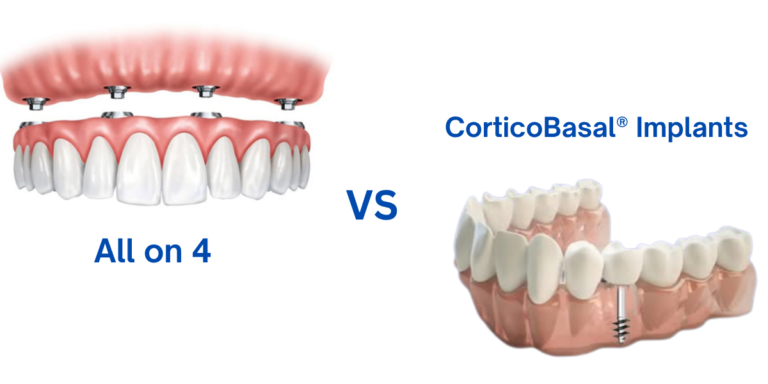
Corticobasal implants differ fundamentally from conventional implant systems in their anchorage strategy.
Instead of relying primarily on cancellous (spongy) bone, corticobasal implants are designed to engage dense cortical bone layers, including basal bone structures that are less prone to resorption.
Key conceptual differences include:
Anchorage in cortical bone rather than alveolar bone alone
Reduced dependence on bone grafting
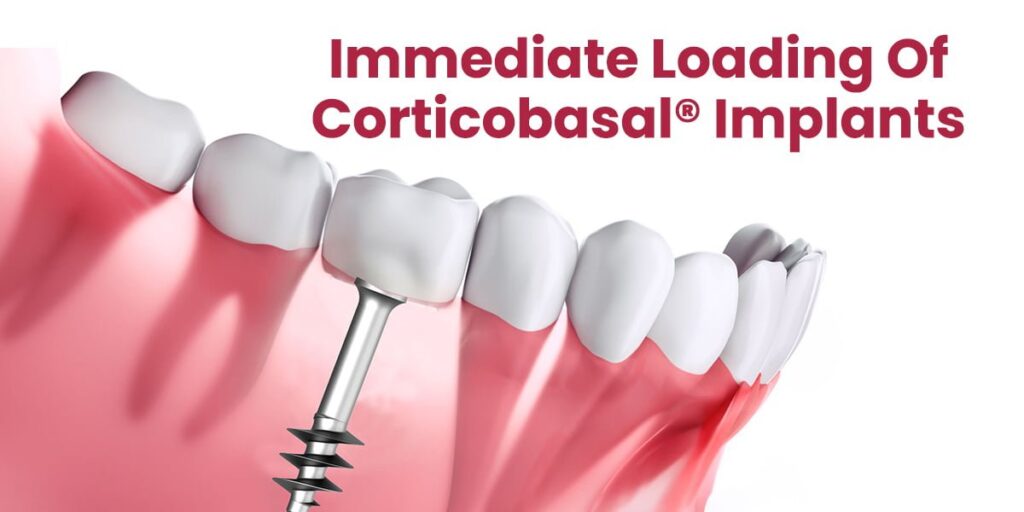
Possibility of immediate or early functional loading in selected cases
Single-piece implant designs in many systems
It is important to note that corticobasal implants are not a replacement for conventional implants but represent a different biomechanical approach altogether.
Where Corticobasal Implants May Be Clinically Relevant
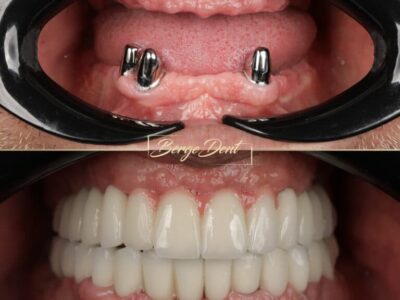
From a practice standpoint, corticobasal implants are typically considered in specific, carefully selected situations, such as:
Advanced ridge resorption where grafting is not feasible
Full-mouth rehabilitation requiring immediate function
Patients who decline sinus lift or augmentation procedures
Cases where treatment time must be minimized
Certain medically compromised patients (with appropriate precautions)
In these scenarios, the ability to anchor implants in stable cortical bone can offer a viable alternative — provided the clinician has the necessary training and experience.
Limitations and the Learning Curve (An Honest Discussion)
One of the reasons corticobasal implantology remains controversial is the steep learning curve involved.
Clinical limitations include:
Highly technique-sensitive surgical protocols
Critical importance of prosthetic planning
Limited margin for error in implant positioning
Need for advanced occlusal understanding
Incompatibility with some conventional workflows
Without structured training and mentorship, attempting such cases can lead to complications. This is why corticobasal implants should be viewed as an advanced clinical skill, not a shortcut.
Making the Right Clinical Decision as a Modern Practice
For dental clinic owners and implant dentists, the real question is not “Are corticobasal implants good or bad?” — but rather:
“Do they make sense for my clinical scope, patient profile, and experience level?”
Sound decision-making involves:
Understanding multiple implant philosophies
Selecting techniques based on case requirements, not trends
Communicating transparently with patients
Avoiding overpromising outcomes
Investing in education before adoption
Dentistry today rewards clinicians who can adapt responsibly, not impulsively.
Expert Perspective: Clinical Insight from Experience
These questions and decisions are best understood through real clinical exposure and case-based learning.
Clinicians like Dr. Madhusudan Krishna, an experienced implantologist, educator, and consultant at Diva Dental Clinic, emphasize and offers advanced dental implant solutions.
With years of hands-on experience in complex implant cases, such expert perspectives help dentists move beyond online opinions and into practical, evidence-informed decision-making.
Why These Conversations Matter Now
 Implant dentistry is no longer about mastering a single system or technique. It is about:
Implant dentistry is no longer about mastering a single system or technique. It is about:
Understanding evolving treatment options
Matching techniques to patient realities
Staying clinically relevant in a competitive environment
Making ethical, informed treatment choices
Platforms like DentCircle exist to encourage open, peer-driven discussions around such evolving topics — without marketing noise or unrealistic claims.
Conclusion
Approach that can be valuable in the right hands, for the right cases.
For modern dental practices, the goal should not be rapid adoption, but informed understanding. When dentists invest time in learning why and when a technique works, patient outcomes — and professional confidence — naturally improve.